Wisdom teeth, also known as third molars, are the last set of molars that most people get in their late teens or early twenties. These teeth are a bit of a mystery to many because they often cause problems and need to be removed. But what exactly is the purpose of wisdom teeth? Are they important to keep, or is it better to have them removed? This article will explore the role of wisdom teeth, why they are often no longer needed, and the reasons behind their removal.
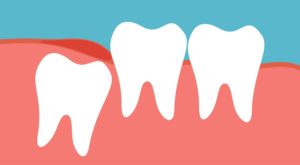
Do Wisdom Teeth Serve Any Purpose?
In the past, wisdom teeth played a crucial role in our ancestors’ diets. Early humans had a diet that consisted of rough food like roots, nuts, and meat, which required a lot of chewing. According to North Tarrant OMS, wisdom teeth were useful for grinding down this tough food, especially when other teeth had worn out or fallen out.
However, today’s diet is much softer and more processed, reducing the need for these extra molars. Modern dental hygiene practices have also improved, allowing people to keep their teeth healthier for longer. As a result, the function of wisdom teeth has become less critical, leading many experts to consider them vestigial organs—body parts that have lost their original function through evolution.
Why Are Wisdom Teeth No Longer Needed?
Wisdom teeth are often no longer needed due to changes in diet and advances in dental care. Over time, human jaws have become smaller because we don’t need as much chewing power. This evolutionary change means that there is often not enough room in the mouth for wisdom teeth to come in properly. North Tarrant OMS explains that as our diets became softer and cooking techniques improved, the need for extra chewing power diminished, leading to smaller jaws.
Additionally, the benefits of dental hygiene, such as regular brushing and flossing, have reduced tooth decay and loss, which were more common in our ancestors. As a result, the space once required for wisdom teeth has shrunk, and these teeth often become impacted or misaligned when they try to emerge.
Are Wisdom Teeth Important to Keep?
While wisdom teeth are not necessary for modern-day chewing or eating, some people may still choose to keep them if they come in properly and do not cause any problems. Dr. Eric Duncan mentions that keeping wisdom teeth can help maintain the natural structure of the mouth. In some cases, they can act as an additional set of molars, providing extra chewing surface.
However, this is relatively rare. Most people experience some issues with their wisdom teeth, such as impaction, infection, or crowding, which can lead to more serious dental problems. Therefore, while it is possible to keep wisdom teeth if they are healthy and properly aligned, it is not always recommended.
What Are the Benefits of Leaving Wisdom Teeth?
If wisdom teeth come in correctly and are healthy, there can be benefits to leaving them in place. One benefit is that they can serve as a backup if other molars are lost due to decay or injury. They can also help maintain jaw structure and support adjacent teeth.
However, these benefits are only applicable if the wisdom teeth are not causing any issues. According to Dr. Eric Duncan, keeping wisdom teeth can sometimes prevent future dental issues by filling gaps left by other teeth and helping with overall mouth structure. But if wisdom teeth are problematic, the risks often outweigh the benefits.
Why Do Dentists Always Want to Remove Wisdom Teeth?
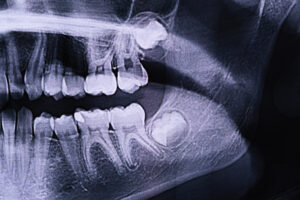
Dentists often recommend removing wisdom teeth to prevent potential problems. Since many people’s mouths do not have enough space for these teeth, they can become impacted, meaning they are trapped beneath the gums and unable to emerge properly. Impacted wisdom teeth can cause pain, infection, and damage to adjacent teeth. WebMD notes that impacted wisdom teeth can lead to cysts, which can damage the jawbone and nerves.
Moreover, even if wisdom teeth do emerge, they can be difficult to clean because they are located so far back in the mouth. This can lead to cavities and gum disease. Dentists often prefer to remove wisdom teeth before they cause these complications, which is why removal is commonly recommended.
What Happens If You Don’t Pull Wisdom Teeth?
If you choose not to pull wisdom teeth, it is essential to monitor them regularly for any signs of problems. Some people never experience issues with their wisdom teeth and can keep them without any trouble. However, for others, not removing wisdom teeth can lead to several complications.
Impacted wisdom teeth can cause pain, infection, and damage to other teeth. They can also lead to overcrowding, making it difficult to maintain proper oral hygiene. According to NCBI, untreated wisdom teeth can result in cavities, gum disease, and cysts. If these problems occur, you may end up needing more extensive dental work in the future.
What’s the Point of Getting Your Wisdom Teeth Pulled?
Getting your wisdom teeth pulled can prevent a range of dental issues. By removing these teeth before they cause problems, you can avoid pain, infection, and damage to other teeth. Additionally, extraction can prevent overcrowding and help maintain proper alignment of your teeth.
Having wisdom teeth pulled is often seen as a preventive measure. It is easier to remove wisdom teeth before they become problematic, and recovery is typically quicker and less complicated when done at a younger age. MyHealth Alberta notes that removing wisdom teeth can help prevent future dental problems and make it easier to maintain good oral hygiene.
Conclusion
While wisdom teeth once served a crucial role for our ancestors, they are largely unnecessary in modern times. Changes in diet and advancements in dental care have made these third molars less relevant, and they often cause more harm than good. Although some people can keep their wisdom teeth without issues, many experience problems such as impaction, infection, and overcrowding, leading dentists to recommend their removal.
By understanding the potential complications associated with wisdom teeth and following the advice of your dental care provider, you can make informed decisions about whether to keep or remove these teeth. Regular dental check-ups and good oral hygiene practices are essential for maintaining overall dental health, regardless of the status of your wisdom teeth.