If you’re thinking about getting veneers or already have them, you might wonder if they can get cavities. Veneers are a great way to improve the look of your smile, but they don’t make your teeth invincible. Let’s break down everything you need to know about cavities and veneers.
Can Veneers Get Cavities?
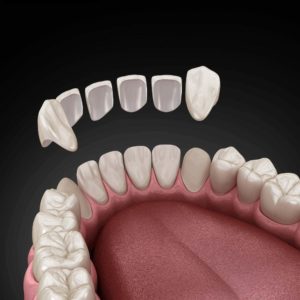
No, veneers themselves do not get cavities. They are made of porcelain or composite resin, materials that do not decay like natural teeth. However, the teeth underneath your veneers are still vulnerable to cavities if they are not properly cared for.
How Do You Know If You Have a Cavity Under a Veneer?
Since veneers cover the front surface of your teeth, spotting a cavity underneath them can be tricky. Here are some signs that may indicate a cavity under a veneer:
- Tooth Sensitivity – If you feel pain or sensitivity when eating hot, cold, or sweet foods, there may be a cavity forming underneath.
- Discoloration – A dark or yellowish stain around the edges of your veneer could mean decay underneath.
- Pain or Discomfort – Persistent tooth pain could indicate a cavity forming behind the veneer.
- Bad Breath – Decay can cause bacteria buildup, leading to bad breath that doesn’t go away with brushing.
- Loose Veneer – If a veneer starts to feel loose or wobbly, a cavity may be damaging the underlying tooth structure.
If you notice any of these symptoms, visit your dentist as soon as possible.
What Happens If You Get a Cavity With Veneers?
If you develop a cavity in a tooth with a veneer, your dentist will need to treat it. The process may include:
- Removing the Veneer – In some cases, the dentist will take off the veneer to access the decay underneath.
- Filling the Cavity – The decayed part of the tooth is cleaned out and filled just like a regular cavity.
- Placing a New Veneer – If the old veneer was removed, a new one may need to be placed.
- Possible Crown Placement – If the decay is too severe, the tooth may require a dental crown instead of a veneer.
Ignoring a cavity under a veneer can lead to more serious dental issues, such as infections or even tooth loss.
Do Teeth Decay Under Veneers?
Yes, teeth can still decay under veneers if proper oral hygiene is not maintained. Here’s how decay can happen:
- Plaque and Bacteria Build-Up – If food particles get trapped around the edges of the veneer, bacteria can cause decay.
- Poor Oral Hygiene – Not brushing and flossing properly can allow cavities to form.
- Gum Recession – If the gums recede, the exposed part of the tooth (not covered by the veneer) becomes vulnerable to decay.
- Weak Bond Between Veneer and Tooth – If a veneer is not properly bonded, bacteria can sneak in and start breaking down the natural tooth.
How to Avoid Cavities Under Veneers
Good oral hygiene is key to preventing cavities under veneers. Here are some tips to keep your teeth and veneers in top shape:
- Brush Twice a Day – Use fluoride toothpaste and brush for at least two minutes.
- Floss Daily – Flossing removes food particles and plaque that brushing can’t reach.
- Use Mouthwash – An antibacterial mouthwash can help kill bacteria and prevent plaque buildup.
- Visit Your Dentist Regularly – Regular checkups allow your dentist to catch any early signs of decay.
- Avoid Sugary Foods and Drinks – Sugar feeds bacteria, leading to cavities. Cut back on sweets and soda.
- Drink Plenty of Water – Water helps wash away food particles and bacteria.
- Avoid Hard or Sticky Foods – These can damage veneers or get stuck between your teeth.
Final Thoughts
While veneers themselves do not get cavities, the natural teeth beneath them can still decay. Taking care of your oral health is the best way to keep your smile looking great and cavity-free. Regular dental visits, good hygiene, and healthy eating habits will help you maintain your veneers and protect your natural teeth for years to come. If you experience any issues, don’t wait—see your dentist right away!